Blog & Resources
Explore our latest articles, guides, and wellness resources below
Peak Interactive Wellness in Denver offers one-day TMS for treatment-resistant depression using the Ampa One system — a full 20-session course in a single day. Serving the Denver, Vail, Breckenridge, Keystone, and Evergreen ares.
4/19/26

Peak Interactive Wellness in Denver offers next-generation interventional psychiatry including one-day TMS with the Ampa One system, ketamine-assisted psychotherapy, and Spravato.
4/13/26

Peak Interactive Wellness in Denver offers comprehensive psychiatric services: evaluations, medication management, ketamine therapy, Spravato, telehealth, perinatal psychiatry, and more.
4/02/26

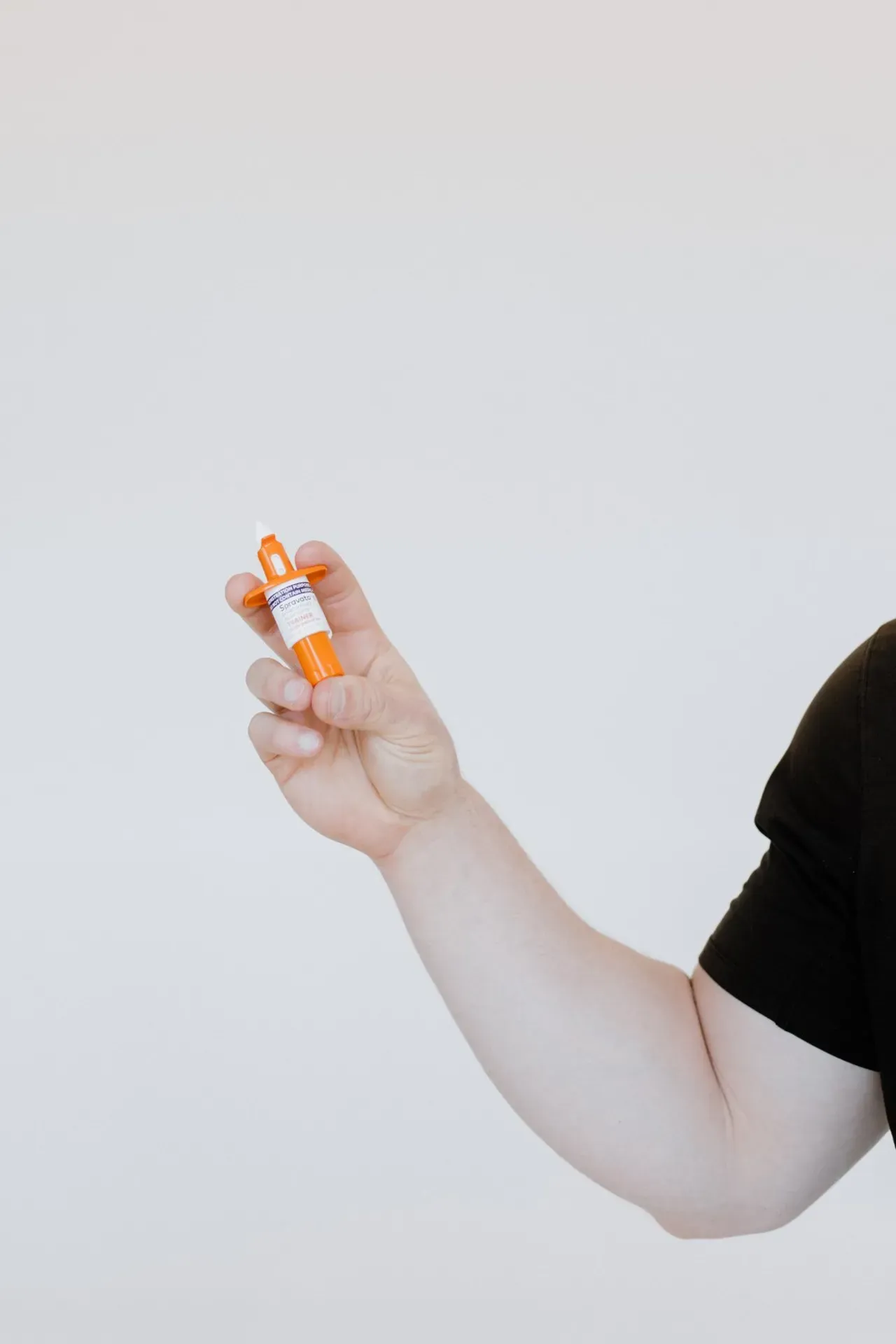
If you’ve tried antidepressants without success, Spravato may help. This FDA-approved esketamine therapy works quickly—often within days—and is delivered safely in a comfortable, monitored setting.
3/22/26

International Women’s Day highlights the importance of women’s mental health. Learn how hormonal changes, life transitions, and societal pressures impact women’s mental health.
3/05/26

Set meaningful mental health goals for the 2026 Year of the Horse with a holistic psychiatry approach. Tips from a Denver psychiatry practice to support mind-body wellness using holistic mental health goals.
2/16/26

Struggling with winter blues or Seasonal Affective Disorder? Learn evidence-based ways to boost your mood this winter and discover compassionate, personalized psychiatric care at Peak Interactive Wellness.
12/12/25

Learn how to build a positive, collaborative relationship with your mental health provider. Explore care at Peak Interactive Wellness in Denver and Greenwood Village, offering holistic psychiatry, therapy, and Spravato®.
12/12/25

Learn what happens during an appointment with a holistic psychiatric nurse practitioner. Discover our integrative, whole-person approach to mental health care at Peak Interactive Wellness in Denver and Greenwood Village.
12/07/25

A clear, patient-friendly guide to taking psychiatric medications safely and effectively. Learn when to take them, how they work, and what to expect. Provided by Denver’s trusted psychiatry experts at Peak Interactive Wellness.
12/07/25

Experience in-person or telehealth couples therapy in Denver with trained Gottman therapist Wendy Tran. 90-min sessions $230 initial | $200 follow-up. No insurance accepted.
11/10/25

Explore SPRAVATO® (esketamine) treatments in Denver, CO for treatment-resistant depression. Learn how it works, who qualifies, and what to expect at Peak Interactive Wellness.
11/10/25
Feeling overwhelmed before the holidays? Discover practical ways to support your mental health with Peak Interactive Wellness in Denver, CO. Mindfulness, gratitude, and stress relief tips from compassionate psychiatry providers.
11/03/25
Discover how simple breathwork techniques reduce stress, calm anxiety, and improve focus. Learn how Peak Interactive Wellness in Denver, CO integrates holistic tools like breath work into personalized psychiatry care.
11/03/25

Discover three key supplements — Omega-3 fatty acids, Vitamin D, and Magnesium — that recent research links to mood, cognition and stress resilience. Learn how to integrate them into a holistic, person-centered mental-wellness plan.
11/03/25

Discover the benefits of ketamine-assisted psychotherapy (KAP) in Denver. Explore how both one-on-one and group KAP sessions can support healing from depression, anxiety, and trauma through a compassionate, holistic approach.
10/23/25

Explore holistic mental health options—from mind-body practices and nutrition to herbal support and acupuncture. Learn evidence-based strategies to nurture emotional wellbeing, resilience, and lifelong mental health.
10/20/25

Learn about ADHD symptoms, natural coping strategies, and Creyos ADHD testing now available at Peak Interactive Wellness in Denver and Greenwood Village. Holistic care that fits your life.
10/19/25

Feeling low as the seasons change? Learn how to manage seasonal depression naturally with simple at-home strategies—and when to reach out for professional help in Denver.
10/17/25

Discover how Spravato™ offers fast-acting relief for depression in Denver. Learn how it differs from traditional antidepressants at Peak Interactive Wellness.
10/14/25

Discover five expert tips for building a fulfilling meditation practice. Learn how mindfulness supports your mental well-being with Peak Interactive Wellness.
10/14/25

Discover how dancing, singing, creativity, and mindfulness can expand your somatic window of tolerance and transform your emotional well-being.
10/13/25

Learn the five most important questions to ask your psychiatric provider. Build a personalized, collaborative mental health plan with Peak Interactive Wellness in Denver.
10/09/25

Discover perinatal mental health care in Denver & Greenwood Village. Peak Interactive Wellness offers telehealth, therapy, and holistic support for new parents.
10/08/25
